Recovery Policy: A Practical Guide to Recovery-Oriented Systems of Care for Policy Makers
Caroline Beidler, MSW is an author, speaker, and the Managing Editor of Recovery.com. She writes about topics related to addiction, mental health, and trauma recovery, informed by her personal experience and professional expertise.

Caroline Beidler, MSW is an author, speaker, and the Managing Editor of Recovery.com. She writes about topics related to addiction, mental health, and trauma recovery, informed by her personal experience and professional expertise.
Table of Contents
- Why This Matters to Policymakers
- Core Pillars of a Recovery-Oriented System of Care (ROSC)
- Frameworks Policymakers Can Use
- Legislative and Administrative Levers
- Barriers to Implementation
- Future-Proofing Recovery Policy
- Strategic Next Steps for Public Officials
- A Recovery System Is the Long Game of Public Health
- How Recovery.com Can Help
In 1976, Operation Understanding broke new barriers and helped change the recovery movement forever. Now, 50 years later, we’re honoring that legacy—and building what comes next.
Part of this effort is sharing the latest evidence-based information on topics that are important to you.
This toolkit was created in partnership with Mobilize Recovery and Recovery.com for Operation Understanding.
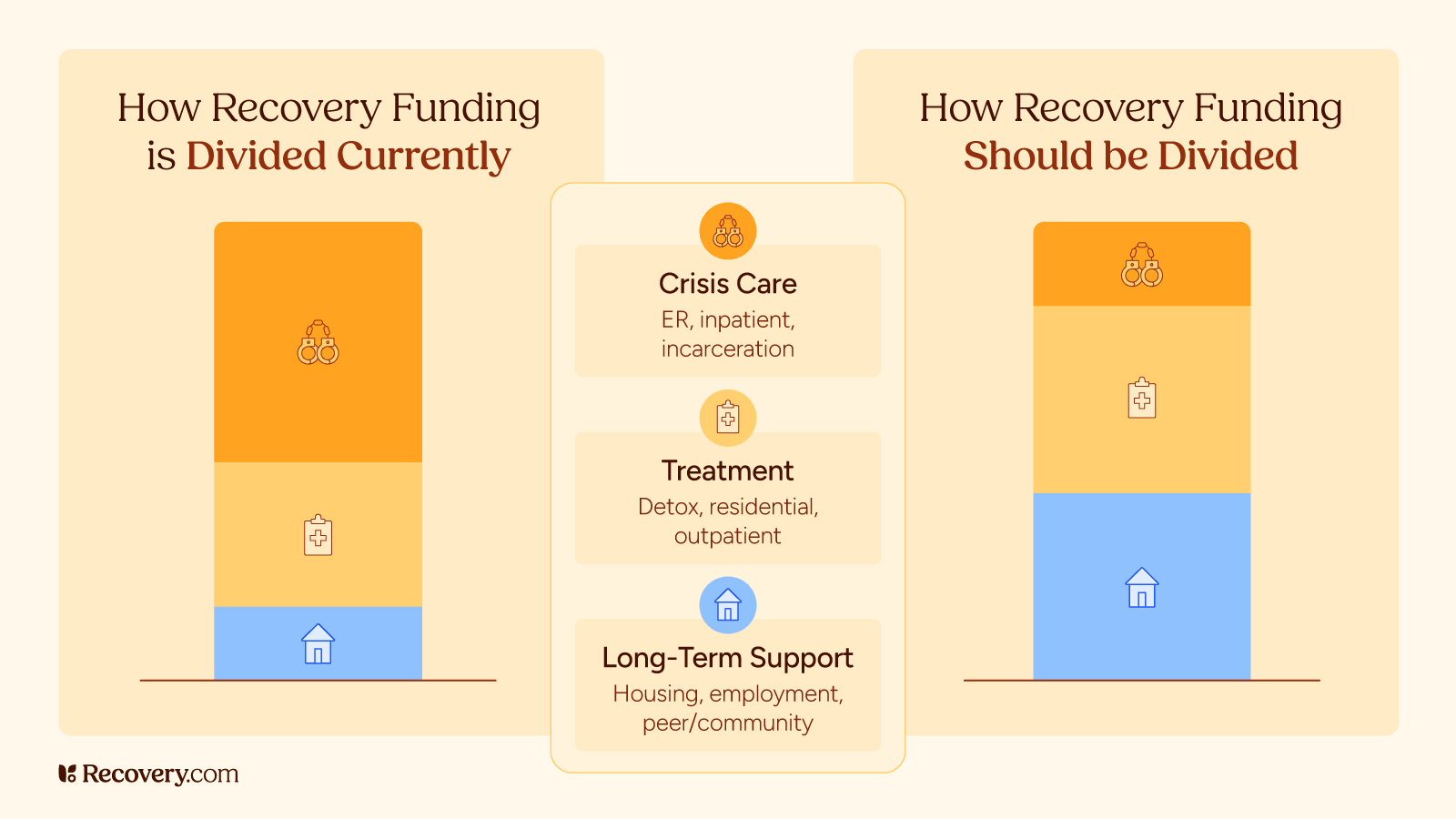
For decades, public policy has treated addiction and mental health as short-term crises to manage. That approach stabilizes people in the moment, but often fails to support what happens next.
A recovery-oriented approach shifts the goal: not just preventing immediate harm, but helping people build stable, healthy lives over time.1 This means aligning health care, public services, and policy decisions around long-term recovery, well-being, and community integration, not just short-term outcomes.
Why This Matters to Policymakers
Recovery policy is not just a health issue. It’s a systems issue that affects budgets, workforce participation, housing stability, and public safety.
When people cycle repeatedly through emergency rooms, jails, and crisis services, costs rise, and outcomes stay the same. Policies that support long-term recovery reduce strain on public systems, improve community well-being, and create measurable returns across multiple sectors.
The economic case: the costs are upstream and downstream
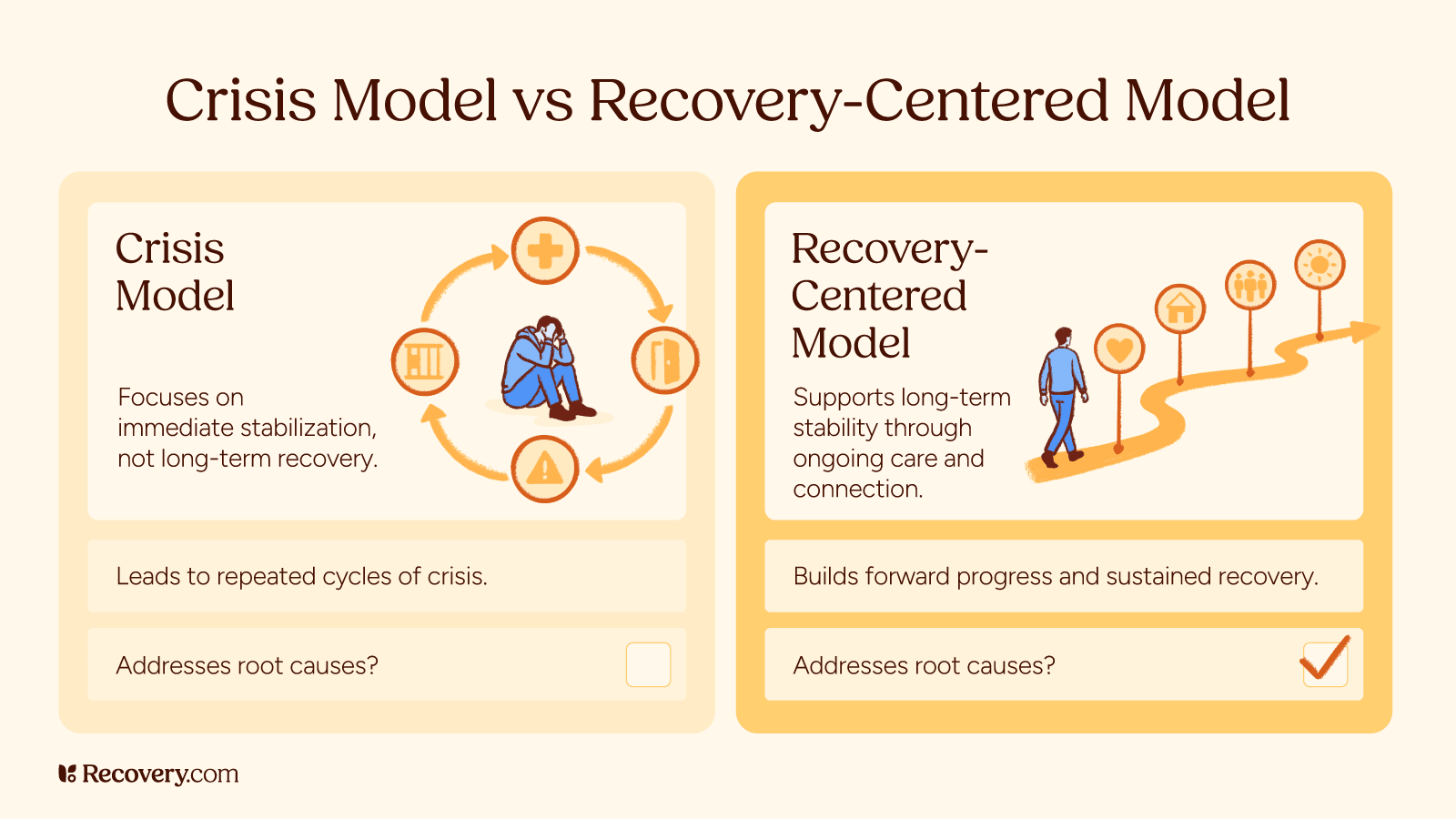
The crisis-first model is expensive because it relies on high-cost settings: emergency departments, inpatient beds, ambulance services, and incarceration. When recovery support is missing, people cycle back through those systems again and again.
Recovery-oriented investments can reduce those costs by improving stability.4 The return isn’t only fewer ER visits. It includes reduced child welfare involvement, lower recidivism, decreased infectious disease transmission, and improved workforce participation. In other words, recovery policy is a financial strategy as much as a moral one.
The human capital case: recovery strengthens communities
Substance use disorder and untreated mental health conditions remove people from the workforce and strain families. When health care systems and public services help people reconnect to purpose (e.g., jobs, education, and meaningful roles) communities gain back capacity.2
This is also where partnerships matter. Employers, workforce programs, schools, and faith communities can become stakeholders in long-term recovery when policy creates practical pathways for reintegration.


Core Pillars of a Recovery-Oriented System of Care (ROSC)
A Recovery-Oriented System of Care (ROSC) shifts the focus from “fix and release” to “treat, connect, and sustain.” A ROSC is a connected network that includes mental health providers, recovery support organizations, and community institutions working toward shared outcomes. This approach aligns policy goals with outcomes like stability, continuity of care, and quality of life.3
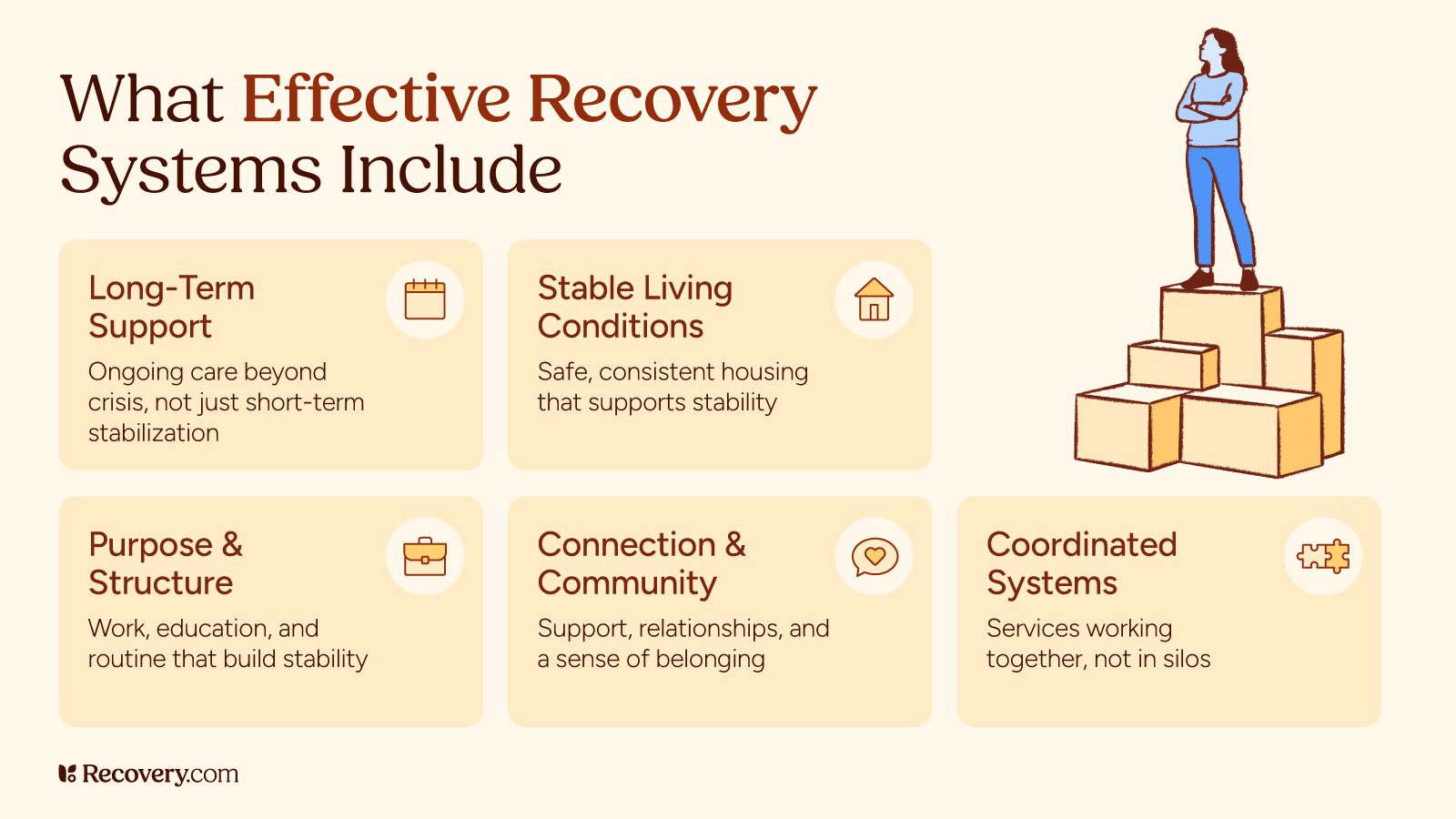
Strong recovery policy typically includes these pillars:
1) Person-led planning and shared decision-making
One-size-fits-all approaches often fail because recovery is deeply personal. Effective initiatives support self-direction, shared decision-making, and individualized goals—whether that means reunifying with family, returning to school, or stabilizing housing.
2) Supports beyond clinical treatment
Treatment alone rarely holds if a person returns to unsafe or unstable conditions. Recovery-oriented systems connect health care to real-life supports such as:
- recovery housing and stable home environments
- transportation
- childcare
- nutrition assistance
- legal aid and reentry services
These supports are not “extra.” They are often the difference between stability and long-term, sustained recovery and recurrence of use or further challenges.
3) Community infrastructure and social connection
Recovery grows in community, through relationships and belonging. Recovery Community Organizations, peer networks, and local coalitions help reduce isolation and strengthen accountability. These networks also reduce stigma, which remains one of the biggest policy issues holding communities back.
Frameworks Policymakers Can Use
Practical frameworks guide decision-making, funding, and evaluation. The following includes helpful frameworks that help translate recovery into measurable outcomes.
SAMHSA’s guiding dimensions
SAMHSA offers a widely used lens for understanding recovery across four dimensions: Health, Home, Purpose, and Community.6 Policymakers can use these as a simple filter for evaluating proposals:
- Does this improve health and access to mental health services?
- Does this strengthen home stability and safe housing?
- Does this create purpose through work, education, or daily structure?
- Does this build community support and relationships?
Recovery capital as a policy metric
Recovery capital refers to the internal and external resources that help someone start and sustain long-term recovery. It includes:
- personal resources (health, finances, skills)
- social resources (family support, healthy relationships)
- community resources (accessible services, low stigma, recovery-friendly environments)
This framework helps translate recovery policy into measurable outcomes that can guide initiatives, budgeting, and accountability.
Measuring quality of life, not only abstinence
Many systems still measure success mostly through “clean time.” That’s too narrow. High-quality measurement also includes quality-of-life indicators like housing stability, employment, reduced justice involvement, physical health improvement, and family stability.5

Legislative and Administrative Levers
Policy change requires coordination across systems. Funding, Medicaid alignment, and workforce development are key levers.
Funding mechanisms: coordinating across silos
One major barrier is fragmentation: health, housing, justice, and labor funding often sit in separate buckets. Recovery policy can support braiding and pooling resources so programs work as a coordinated system rather than disconnected services.
Medicaid and health policy alignment
Medicaid is often one of the most powerful levers for expanding recovery support, especially for peer services and community-based supports.7 When Medicaid coverage includes non-clinical recovery support, continuity improves and costs often fall over time.
Peer support and workforce standards
Peer Support Specialists or people with lived experience who are trained to support others are a critical bridge between clinical providers and daily life. Policy can strengthen the peer workforce through certification standards, reimbursement pathways, and sustainable funding for support services.

Barriers to Implementation
System fragmentation, stigma, and data challenges limit progress. Addressing these barriers improves outcomes and efficiency.
- Siloed systems across agencies: People with substance use disorder and mental health needs may touch multiple systems like public health, courts, housing, schools, workforce development, yet those systems often don’t share information or coordinate plans. Cross-agency coordination and shared strategy can reduce gaps and improve outcomes.
- Stigma as a policy barrier: Stigma shows up as resistance to recovery housing, restrictive licensing, and hiring discrimination.8 Advocacy from leaders can shift culture, but policy changes like fair chance hiring and zoning protections also matter.
- Privacy and data sharing: Federal rules (including 42 CFR Part 2) exist to protect privacy, but they can complicate coordination.10 The goal is not to weaken privacy, but to build secure data-sharing agreements that allow continuity while protecting rights.
Future-Proofing Recovery Policy
Sustainable policy must adapt to technology, expand access, and include lived experience in decision-making.
- Technology, access, and the pandemic lesson: The pandemic accelerated telehealth and remote recovery support. Keeping those tools available and reimbursable can expand access in rural areas and reduce barriers for people with transportation or childcare limitations. This is a practical public health gain.
- Stakeholders and “nothing about us without us”: High-quality policy improves when people with lived experience have real influence. That means more than listening sessions. It means seats on boards, advisory councils, and program design teams. When stakeholders include lived experience voices, policy choices are more realistic and outcomes improve.
Strategic Next Steps for Public Officials
Actionable steps help translate strategy into impact. Long-term planning and partnerships are essential.
Run a recovery resource audit
Map what exists and what’s missing. Many communities find they have plenty of crisis services but limited long-term supports like housing, peer networks, and employment pathways.
Build a multi-year recovery roadmap
Recovery policy is not a single bill. It’s a sustained strategy that should survive political cycles—across local government and federal government changes—by focusing on stable goals, measurable outcomes, and durable partnerships.
Strengthen coalitions and partnerships
Bring together mental health providers, public health agencies, recovery community organizations, hospitals, employers, universities, and advocacy groups. Coalitions help coordinate initiatives, reduce duplication, and improve continuity.
These steps create alignment, reduce duplication, and improve long-term outcomes.
A Recovery System Is the Long Game of Public Health
Recovery-oriented policy is a commitment to the long game: fewer cycles through crisis systems, stronger families, a healthier workforce, and communities with greater well-being. It requires clear decision-making, honest assessment of trade-offs, and sustained investment in recovery support.
Policymakers can shape this future through health policy, Medicaid decisions, partnerships with federal agencies, and coordinated initiatives that treat recovery as a community outcome, not just an individual struggle. When we build systems that support long-term recovery, we don’t only save lives. We strengthen the whole fabric of public health.
Additional Resources
Check out these additional peer-reviewed sources for more information about recovery policy.
- Centers for Disease Control and Prevention. (2025, June 10). Strategic priorities for overdose prevention. https://www.cdc.gov/overdose-prevention/strategic-priorities/index.html
- Centers for Disease Control and Prevention. (2025, August 26). National Recovery Month partner toolkit. https://www.cdc.gov/overdose-prevention/php/toolkits/national-recovery-month.html
- Substance Abuse and Mental Health Services Administration. (2026, March 11). About recovery. https://www.samhsa.gov/substance-use/recovery/about
- Substance Abuse and Mental Health Services Administration. (2026, March 23). Peer support workers for those in recovery. https://www.samhsa.gov/substance-use/recovery/peer-support-workers
- U.S. Department of Health and Human Services. (2024, February 8). Fact sheet: 42 CFR part 2 final rule (Updated January 30, 2026). https://www.hhs.gov/hipaa/for-professionals/regulatory-initiatives/fact-sheet-42-cfr-part-2-final-rule/index.html
- National Academies of Sciences, Engineering, and Medicine, Health and Medicine Division, Board on Health Care Services, Committee on Strategies to Improve Access to Behavioral Health Care Services through Medicare and Medicaid, Perera, U., Godwin, A., & Polsky, D. (Eds.). (2024). Expanding behavioral health care workforce participation in Medicare, Medicaid, and marketplace plans: The U.S. behavioral health care system (Chapter 3). National Academies Press. https://www.ncbi.nlm.nih.gov/books/NBK609446/
- National Institute on Drug Abuse. (n.d.). Recovery. https://nida.nih.gov/research-topics/recovery
- National Institute on Drug Abuse. (n.d.). Stigma and discrimination. https://nida.nih.gov/research-topics/stigma-discrimination
- National Institute on Drug Abuse. (n.d.). Substance use disorders. https://nida.nih.gov/research-topics/substance-use-disorders
- Recovery Research Institute. (2024, February 22). Recovery community centers: Is participation in these newer organizations associated with better outcomes? https://dev.recoveryanswers.org/research-post/recovery-community-centers-associated-with-well-being/
- Recovery Research Institute. (2024, February 22). Study of recovery community organization participants over time shows peer-based recovery support activities are associated with modest improvement in recovery capital. https://dev.recoveryanswers.org/research-post/study-recovery-community-organization-participants-peer-based-recovery-support-mod...
- Substance Use & Misuse. (2025). Recovery capital is associated with a greater likelihood of NIAAA-defined recovery for adults with prior alcohol problems [Abstract]. https://pubmed.ncbi.nlm.nih.gov/40165402/
How Recovery.com Can Help
Recovery.com is a free, impartial treatment navigation platform that helps people find evidence-based addiction and mental health care quickly, with clinically reviewed content, transparent center profiles, and tools designed to enhance treatment access.
This toolkit was created in collaboration with Mobilize Recovery for Operation Understanding.
FAQs
A recovery-oriented system of care (ROSC) is a coordinated network of services that supports long-term recovery from substance use disorder and mental health conditions. Instead of focusing only on crisis care, it connects patients to housing, employment, community support, and ongoing treatment to help them build stable, meaningful lives.
Crisis-based care focuses on short-term stabilization, like emergency treatment or inpatient stays. While this can save lives, it often doesn’t address the underlying factors that contribute to relapse, such as unstable housing, trauma, or lack of support. Without continued care and resources, many patients return to the same challenges that led to the crisis.
Effective recovery policy includes person-centered care, access to mental health services, and support beyond treatment—like housing, employment, and peer networks. It also relies on coordination between public health systems, community organizations, and policymakers to create lasting outcomes.
Recovery policy strengthens communities by reducing emergency service use, lowering incarceration rates, and improving workforce participation. When patients have the support they need to maintain recovery, families stabilize, local economies grow, and public health outcomes improve.
Lived experience provides real-world insight into what recovery actually requires. When policymakers include people in recovery in decision-making, policies are more practical, effective, and responsive to community needs. This approach helps ensure that services truly support long-term recovery, not just short-term outcomes.
Our Promise
How Is Recovery.com Different?
We believe everyone deserves access to accurate, unbiased information about mental health and recovery. That's why we have a comprehensive set of treatment providers and don't charge for inclusion. Any center that meets our criteria can list for free. We do not and have never accepted fees for referring someone to a particular center. Providers who advertise with us must be verified by our Research Team and we clearly mark their status as advertisers.
Our goal is to help you choose the best path for your recovery. That begins with information you can trust.